I agreed, which didn’t seem to satisfy him at all. So let me explain further in this blog, as it will take longer than a passing corridor conversation, unless you have the old Victorian corridors still, I may be able to explain it in the time it takes to walk one of those, ah the days when we all got more exercise at work.
|
I was walking down the corridor when one of the Medical Registrars walked passed looking perplexed, we said hello and passed on by, then he called after me “oh can I ask your opinion on…” A standard start to many a query for a Microbiologist! But this question was different, he was reading around the subject of endocarditis and was frustrated by the “guidelines” put out there by the expert bodies… he went on “their advice is sometimes different and even contradictory! How do you know what to follow?”
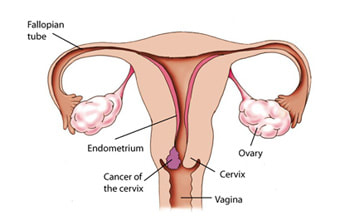
I agreed, which didn’t seem to satisfy him at all. So let me explain further in this blog, as it will take longer than a passing corridor conversation, unless you have the old Victorian corridors still, I may be able to explain it in the time it takes to walk one of those, ah the days when we all got more exercise at work. More than 90% (possibly as high as 99%) of cervical cancer is related to previous infection with human papillomavirus (HPV), also known as the wart viruses. HPV is a double-stranded DNA virus. Viral replication causes changes within cells which can sometimes lead to the cell becoming cancerous. Different types of HPV affect different tissues; some cause warts on hands, some cause warts on feet (verrucas) and some cause anogenital warts (with the slightly over the top medical term, condyloma acuminatum). There are more than 200 different types of HPV, many of which can cause cancer, including oropharyngeal, laryngeal cancer, and sometimes even skin cancers, however perhaps the best known link is to cervical cancer.
The patient was a middle aged man who was originally born in South America, but who had lived in the UK for a number of years. He made an appointment to see his GP when his wife had noticed that his eyes had started to go yellow. By the time he saw his GP he was clearly jaundiced, although he was not febrile and had no abdominal pain and so infection was not suspected. The GP arranged for some blood tests and an abdominal ultrasound scan to look for any obstruction in the biliary system which might account for the man’s symptoms. The blood tests confirmed a raised bilirubin and slightly abnormal live enzymes, but the total white blood cell count and CRP looked normal. The ultrasound did not show any gallstones (the most common cause of obstruction in the UK other than traffic jams!) but did show a dilated common bile duct which suggested some form of obstruction.
On my way around the wards recently I was asked a question that had me stumped. The respiratory doctors were looking after a patient who they thought either had tuberculosis or lung cancer. The patient had a pleural effusion and the doctors asked “what is the test that distinguishes between tuberculosis (TB) and malignancy?”
My first response to this was to talk about microbiology tests such as microscopy and culture but the doctors quickly stopped me waffling on. “No, no” they said, “what’s the biochemistry test?” I didn’t know. I could use the excuse that I’m not a Biochemist but I could see that that was not going to be good enough; I’m a Microbiologist so tuberculosis is in my field of expertise. I clearly had some reading to do! So I made a promise to write a blog on the answer. Well here you go Kate, here’s your blog… and thanks for the question, it’s always great to learn something new… Sometimes you come across an idea so brilliant and yet so simple that you think to yourself “I wish I’d thought of that!” Well that’s what happened to me at the Federation of Infection Societies annual conference at the beginning of December.
I guess I should start by saying I have no affiliation to, or sponsorship from, any company, pharmaceutical or otherwise. I can therefore say I am totally objective, but I was impressed! So what was it I was so impressed by? Well, it’s a beta-lactamase… What, a beta-lactamase!?! But they’re bad, they breakdown antibiotics and stop them working, how can they be a good thing? Well, before we consider the beta-lactamase let’s think about why antibiotics can be bad for you. |
Facebook has deleted the Microbiology Nuts & Bolts pages - if you want your weekly dose of microbiology then you will need to come here, and we look forward to you continuing to read it!
Blog Author:
David Garner Please DO NOT advertise products and conferences on our website or blog
Categories
All
Archives
November 2022
Categories
All
|
 RSS Feed
RSS Feed
