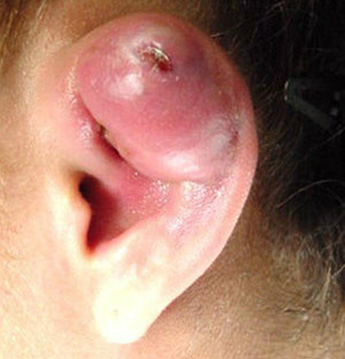
Three days later the patient started to get some pain in her ear and noticed that the top of her ear was starting to swell. She hoped it would settle down but after two more days the pain was severe and the upper part of her pinna was now very swollen and red. She attended the Emergency Department who diagnosed a severe infection of her outer ear, admitted her for IV Flucloxacillin (a great choice normally for skin infections) and removed the ear ring. As the ring was removed a large quantity of pus poured out of the piercing hole. This was collected in a sterile universal container and sent to the microbiology laboratory. A Gram stain of the pus showed lots of Gram-negative bacilli.
|
The patient was 19 years old and had decided to get her ear pierced. She already had pierced ear lobes so thought it would be good to have a ring through the top of her ear. She went to a local tattoo and piercing centre that followed their standard procedure and aseptically introduced a ring through the cartilage of the helix of the patient’s pinna…ouch! All done in the name of self-expression…
Three days later the patient started to get some pain in her ear and noticed that the top of her ear was starting to swell. She hoped it would settle down but after two more days the pain was severe and the upper part of her pinna was now very swollen and red. She attended the Emergency Department who diagnosed a severe infection of her outer ear, admitted her for IV Flucloxacillin (a great choice normally for skin infections) and removed the ear ring. As the ring was removed a large quantity of pus poured out of the piercing hole. This was collected in a sterile universal container and sent to the microbiology laboratory. A Gram stain of the pus showed lots of Gram-negative bacilli. A 3 year old girl was seen in the paediatric outpatient clinic having been referred because of vomiting and diarrhoea associated with iron deficiency anaemia. On examination this small girl looked a little malnourished; she had some mild generalised abdominal discomfort and distension. The paediatrician noted that the patients GP had arranged for a stool culture to be sent to the microbiology laboratory but that the result was still awaited, so the paediatrician rung the duty microbiologist to see if there was anything growing yet … this not something we would normally encourage as preliminary results can be misleading. However rather than just say wait for the results, the Microbiologist checked the child’s blood results and asked for some more information.
The full blood count showed that the child had a very high peripheral eosinophil count in addition to the iron deficiency anaemia. The paediatrician was asked to check if the child had had any respiratory symptoms including a dry cough or wheeze in the last few months. The child’s mother confirmed that the child had a cough and wheeze for a couple of weeks two months ago which had settled of its own accord. “This sounds like ascariasis” commented the Microbiologist. “Surely it can’t be; that only occurs in tropical countries and they haven’t been anywhere” replied the Paediatrician. An elderly man was brought in to see his GP by his son who was concerned about progressive memory loss in his father. The son reported that his father had been getting more forgetful over the past few weeks and he was concerned that this was more than a slow cognitive deterioration related to his age. The GP sent a number of basic tests to the laboratories including haematology and biochemistry tests and also decided to ensure there wasn’t an infective cause by sending urine for culture and a serum sample for syphilis serology.
The result of the syphilis serology came back showing: EIA positive not confirmed in second assay TPPA negative RPR positive Interpretation: EIA and RPR likely to be false positives. Treponemal infection unlikely but please repeat to confirm. The GP stared at the result for a few minutes before rolling his eyes to the ceiling and saying “what does this all mean; why the heck did I do this test?” Good questions! In December 2015 Angola reported an outbreak of yellow fever in Luanda to the World Health Organisation (WHO). Although yellow fever is endemic in Angola the outbreak was of concern as it was occurring in an urban area and therefore had greater scope than usual to spread and involve more people. Since December there have been 3867 reported cases in Angola and 369 suspected deaths. The virus has spread to the Democratic Republic of Congo who have reported a further 2269 cases; and Kenya and China have had related cases in returned travellers. This is a very large outbreak; to put it in context the last outbreak in Angola, in 1988, affected 37 people and caused 14 deaths. The WHO has so far used 18 million doses of vaccine to try and bring the outbreak under control but it's still ongoing.
|
Facebook has deleted the Microbiology Nuts & Bolts pages - if you want your weekly dose of microbiology then you will need to come here, and we look forward to you continuing to read it!
Blog Author:
David Garner Please DO NOT advertise products and conferences on our website or blog
Categories
All
Archives
November 2022
Categories
All
|
 RSS Feed
RSS Feed
