“Of course, what’s the story?” replied the Microbiologist.
“We have a baby who is just over 24 hours old. They were born at term in good condition but started to grunt and looked mottled by 4 hours. We brought them to the Neonatal Unit, did blood cultures and started IV Benzylpenicillin and Gentamicin as per guidelines but they’re not really improving. Do you think we need to change the antibiotics? Has anything grown in the blood culture?”
The Microbiologist chose to ignore the last question as blood cultures are incubated in an automated incubator which scans the bottles every 10 minutes. If the blood culture where positive then it would have been phoned already.
“Is the baby’s mother okay? Have there been any problems during the pregnancy. Was the mother fully vaccinated? Was the labour normal? Is there anything else you’ve noticed about the baby, any odd lumps, bumps or spots?” asked the Microbiologist.
The Microbiologist pricked up their ears.
“Was a scalp electrode placed in labour? Do the bumps look like vesicles and are they close to the site of the electrode?”
“Now you ask, yep a scalp electrode was placed and the lumps are nearby. But so what?”
“Okay, I think this is neonatal Herpes Simplex Virus infection. Can you get a viral swab from one of these lesions? The baby needs to start IV Aciclovir as soon as possible. Does the mother have a history of HSV?”
“The mother has no history of genital herpes, surely it must be something else!” the Registrar said in a frustrated tone…thinking yet another wild goose chase by the Microbiologists, do they not have anything better to do than “make-up” clinical scenarios?
“Nope, it’s not, most reactivation of genital HSV is asymptomatic and therefore it is often not suspected. Get the swabs and start the Aciclovir and then I’ll explain more…”
What is neonatal Herpes Simplex infection?
Neonatal Herpes infection occurs shortly after birth, usually within a few days, caused by genital Herpes Simplex Virus (HSV) acquired from the baby’s mother. Most infection is due to HSV 2 which is the most common cause of genital herpes. HSV 2 infection is more severe than HSV 1 (normally the cause of oral or orolabial herpes infection).
Genital herpes is a sexually transmitted infection which is often asymptomatic but can also presents with painful ulcers. After the primary infection, whether it is treated or untreated, HSV sits latent in the local sensory nerve ganglia from which it can reactivate causing recurrent infection. The majority of reactivation is asymptomatic and shedding of virus can occur at any time. The highest risk of transferring the infection to the baby is with primary genital herpes at the time of delivery (30-50% risk) but it can also occur with asymptomatic reactivation (3% risk). Most neonatal herpes infection occurs in asymptomatic mothers!
Infection transfer usually occurs after the baby swallows or inhales virally infected fluid at the time of delivery (85%) but it can occur in-utero (5%) or postnatally (10%) from genital or orolabial herpes (therefore adults with cold sores should not kiss newborn babies). The incidence of neonatal HSV infection is commonly thought to be 1-2 per 100,000 live births in the UK but may be as high as 17.5 per 100,000 live births.
How does neonatal herpes present?
The problem with diagnosing neonatal herpes is that it presents in the same way as any other type of neonatal infection. Babies are often drowsy, pale, mottled or cyanosed, can have bradycardias or apnoeas (where they stop breathing for a period of time) or may even have seizures. But these are the features of any sick baby and are not specific to neonatal herpes. In order to diagnose neonatal herpes you have to be suspicious of neonatal herpes in ANY sick baby within the first 3-4 weeks of life otherwise you will miss it.
Clues that can help diagnose neonatal herpes include:
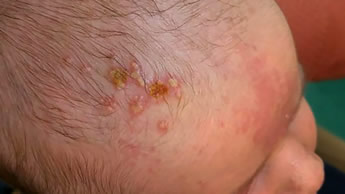
- Vesicles at the site of scalp electrodes – the HSV enters the skin at the site of the break in skin where the scalp electrode was placed; scalp electrodes are used to monitor the pH of the fetus and give an indication of fetal distress if the pH starts to drop (i.e. the fetus is becoming acidotic)
- Raised liver enzymes (aspartate transaminase or alkaline phosphatase) with a coagulopathy (slow blood clotting time) due to liver damage by the virus
There are three main types of clinical infection in neonatal HSV:
- Skin Eye Mouth (SEM) infection (45%), skin vesicles including infection around scalp electrodes or other sites of minor trauma, conjunctivitis and keratitis (inflammation of the cornea)
- CNS infection (30%), including encephalitis, lethargy, fever and seizures
- Disseminated infection (25%), sepsis syndrome with hepatitis, disseminated intravascular coagulation (DIC), low platelets and pneumonitis (any form of disseminated infection can also have the features of SEM and CNS infection)
How do you diagnose neonatal herpes?
The diagnosis of neonatal herpes is based upon demonstrating the presence of HSV by taking viral swabs from skin lesions, nasopharynx, mouth, and conjunctiva as well as taking blood and cerebrospinal fluid (CSF) for HSV PCR.
One of the biggest problems for microbiology and virology laboratories is that not enough CSF is taken to do all the tests requested. Laboratories often get only a few drops in a tube with which to do cell counts, culture and PCR as well as being expected to give some to biochemistry to measure protein! It simply is not enough to do all those tests. Babies produce about 0.35ml/kg/hour of CSF therefore it is safe to take 0.2ml/kg of CSF for testing; for an average birth weight child in the UK (2.5-4kg) this is 0.5-0.8ml (about 10-16 drops).
Non-microbiological tests include a Full Blood Count (FBC), Clotting Screen and Liver Function Test. Magnetic Resonance Imaging (MRI) of the brain and an Electroencephalogram (EEG) are also important to look for brain damage as well as an Ophthalmology review to look for eye disease.
How is neonatal herpes treated?
Neonatal herpes should be treated with high dose (20mg/kg) IV Aciclovir TDS as soon as the diagnosis is suspected and treatment should be started before any results are available. This is because Aciclovir is more effective the earlier it is started.
Aciclovir is a pro-drug; it is not active in its original form but is activated by the virus’s thymidine kinase enzyme. It is not active until the virus is present, but once the virus has caused damage Aciclovir cannot help repair that damage.
The normal IV treatment duration is:
- SEM – 14 days
- CNS or Disseminated – 21 days
A repeat CSF for HSV PCR should be taken before stopping IV Aciclovir in babies with CNS infection and if this remains positive a further week of IV Aciclovir should be given and the CSF repeated again. The IV Aciclovir should be continued until the CSF HSV PCR is negative.
Before the availability of Aciclovir the mortality from neonatal herpes was as high as 75%, with 90% of survivors having long-term neurological damage. With treatment the mortality and long-term complications are related to the type of infection:
Type of infection |
Mortality |
Long-term sequelae |
SEM |
Rare |
2% |
CNS |
4% |
30% |
Disseminated |
30% |
80% |
- Mother: if a mother has active genital herpes at the time of labour they should be started on IV Aciclovir and the baby should be delivered by caesarean section within 4-6 hours of rupture of membranes. This significantly reduces the risk of neonatal herpes but does not completely prevent it; remember 15% of neonatal herpes is not acquired by passage through the genital tract, 5% occurs in-utero or 10% postnatally from genital or orolabial herpes.
- Baby: any baby born (natural or caesarean birth) to a mother with active genital herpes should be started on IV Aciclovir after birth and this should be continued until infection has been ruled out as for the diagnosis of HSV above (swabs and CSF).
- Any baby born to a mother with a history of recurrent genital herpes should have nasopharyngeal, mouth and conjunctival surface swabs taken to look for exposure to the virus and they should be observed for signs of infection until these swabs come back negative. If the surface swabs are positive the baby should have a full screen including blood and CSF; if negative the parents should be warned about the clinical features of neonatal herpes and the urgent need to return to hospital if these occur over the next 4 weeks.
Some experts recommend oral Aciclovir from 36 weeks gestation until after delivery for all mothers with a history of genital herpes infection to prevent the development of active lesions around the time of delivery. The efficacy and safety of this approach are not known but it may be helpful.
What about preventing recurrence in the baby?
Following the initial neonatal herpes infection the virus remains in the sensory ganglia of the nerve cells and can reactivate. This is very common when the initial infection occurred in the neonatal period (birth to 28 days). Between 50-80% of babies will have recurrent episodes of herpes infection in the first year of life with 1-12 episodes per baby; ≥3 episodes in the first 6 months is associated with greater long-term neurological damage.
Because of the risk of recurrence and the damage this can cause, all babies who have had neonatal herpes should be given 6-12 months of oral Aciclovir to prevent such recurrences. This reduces the risk of recurrence but doesn’t completely prevent it from happening so parents need to be aware and return to hospital if symptoms of herpes infection recur.
So our baby was started on IV Aciclovir as soon as the registrar put the phone down. Swabs from the skin lesions confirmed HSV 2 infection but fortunately for the baby the blood and CSF PCRs were normal. They were treated with 2 weeks of IV Aciclovir and sent home on a planned 12 months of oral Aciclovir. At the 1 month review the baby was doing well and no further episodes had occurred. Review as an outpatient will continue for at least 12 months but it is hoped that the baby will be fine in the future.
 RSS Feed
RSS Feed
