PCP is an opportunistic lower respiratory tract infection caused by the fungus Pneumocystis jirovecii (previously known as Pneumocystis carinii, but this name is now used to only describe the species that infects rats!). P. jirovecii is everywhere in the environment, and approximately two thirds of us have acquired it through inhalation by the time we are 2 years old. The micro-organism remains in the lungs (latent) without causing any problem unless we become immunosuppressed for some reason. As the immune system becomes inadequate, e.g. the loss of CD4 lymphocytes in HIV infection (it is an AIDS defining illness) or chemotherapy induced neutropaenia, it no longer holds the organism in check so the fungus becomes active and infection occurs.
Co-Trimoxazole is normally very effective at preventing PCP but there are some problems with its use in pregnancy. Because it is an anti-folate drug it can be associated with congenital birth defects when used in the 1st trimester.
Some doctors give extra supplements of folic acid to try and prevent the development of birth defects however there is evidence that high folic acid supplementation in pregnancy increases the risk to the mother of PCP treatment failure and death. P. jirovecii uses this folic acid to bypass the action of the Co-Trimoxazole. Co-Trimoxazole normally kills bacteria by preventing the bacteria’s synthesis of folic acid but it seems that this fungus can utilise free folic acid for its DNA synthesis therefore it is not killed.
The key to making the diagnosis is having a strong suspicion of PCP in an immunosuppressed patient. There are no definite characteristics however patients tend to have hypoxia which worsens on minimal exertion e.g. walking to the toilet.

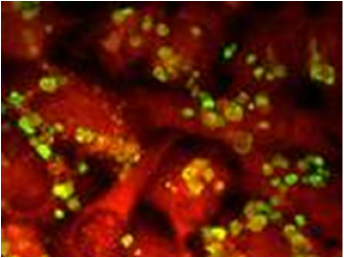
1. Direct staining of Bronchoalveolar lavage (BAL) specimens either using a Silver-Grocott stain in histopathology or immunofluorescence in microbiology
2. Molecular detection of P. jirovecii using PCR on either a BAL sample or an EDTA blood sample
How is PCP treated?
If the diagnosis is suspected then treatment should be started before tests results are confirmed, as most laboratories in the UK don’t have the capability to diagnose PCP quickly. First line treatment of PCP is IV or PO Co-Trimoxazole (Septrin) at high doses, 30mg/kg QDS or 60mg/kg BD, although the dose does need adjusting for renal failure. Co-Trimoxazole is still used to treat even if the patient has been on prophylaxis because the doses used to treat it are much higher than those used to prevent it (typically prophylaxis is with 480mg a day whereas treatment is with 8,400mg a day!). Treatment should be continued for 21 days. The other crucial component of treatment is the use of steroids, normally PO Prednisolone 40mg BD. It is the steroids that save lives in PCP as they damp down the inflammation associated with infection and give enough time for the antibiotics to work. Second line treatment for severe PCP is with Primaquine and Clindamycin, but usually only under the guidance of a specialist in infectious diseases or genitourinary medicine.
• PCP is a severe disease, and it should be considered in any profoundly immunosuppressed patient with a lower respiratory tract infection
• PCP in pregnancy should be treated normally as the benefit of treatment outweighs the risk of harm to the baby
• Investigation takes time and therefore treatment should be initiated as soon as possible
• Even with appropriate treatment the mortality can be as high as 20-40%
For this patient the treatment went well and so far there does not appear to be any problems for her baby.


 RSS Feed
RSS Feed
