“I don’t know what happened” she cried to the Paediatrician, “he was just a bit irritable when I put him to sleep last night and had a bit of redness around his mouth, but this morning his skin is falling off!” She then dissolved into floods of tears.
The Paediatrician took one look at the blisters and broken skin around the baby’s umbilicus and nappy area and asked “could he have been scalded with hot water at all? He looks burnt!
“Okay, this is an infection called Staphylococcal Scalded Skin Syndrome. Let’s get your baby started on antibiotics and send off some tests. We’ll get you both up to the ward and go from there” the Paediatrician said as calmly as possible.
“Is he going to be scarred for life?” the mother asked.
“No, he won’t be scarred for life” said the Paediatrician, whilst thinking that the trauma of the whole thing was likely to mentally scar the baby’s mother for life instead!
Staphylococcal scalded skin syndrome (SSSS), or Ritter disease as it’s also known, is a toxin mediated disease due to the bacterium Staphylococcus aureus. The toxins act on the zona granulosa of the epidermis, interfering with a protein in desmosomes, the organelles that help anchor keratinocytes to each other (I’ve found a picture for you! But essentially keratinocytes are the main cells of the outer layer of skin). This results in the formation of fragile blisters (bullae) that have often broken down by the time the child presents to their family doctor or to the hospital. The result is that the child looks like they has been scalded and is losing their skin.
SSSS is more common in neonates and children than adults, and especially newborn babies, because they do not have a fully developed immune system. They do not have antibodies capable of neutralising the toxin (which adults often develop through exposure later in life) and their renal function is often not good enough to help them pee out the toxins. In adults SSSS tends to only occur in the immunocompromised or those with renal failure for the same reasons as in children, although adult presentation even in these groups is less common.
How does SSSS present?
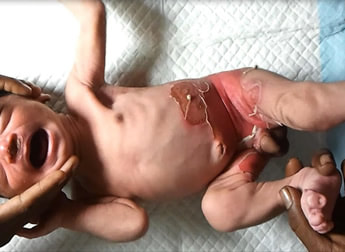
Neonates tend to present 3-7 days after birth. They are usually febrile and irritable. An area of redness develops on the skin (erythema), often either around the mouth or umbilicus, which then becomes blistered 1-2 days later. Blisters also start to form in areas of mechanical stress such as the flexural creases (groin and elbow), hands, feet and buttocks. The blisters then break down leaving areas of underlying raw tissue much like a burn. Infected children can have mucosal hyperaemia (increased blood flow causing redness) which often mimics conjunctivitis.
Like burns, these areas of desquamation are very painful. In fact SSSS looks so much like burns that there is often an initial concern that the child might have been burnt or scalded with hot water and raises concerns of non-accidental injury (child abuse).
An important distinguishing feature of SSSS from the main differential diagnosis of Toxic Epidermal Necrolysis (TEN) is that in SSSS the mucous membranes are not involved. TEN is similar in presentation to SSSS but is a non-infectious drug-induced skin disease which although rare can be life-threatening. If you were to biopsy a lesion, which is rarely necessary, the histology would show sloughing of only the upper layers of the epidermis in SSSS whereas in TEN there is subepidermal splitting and full-thickness epidermal necrosis.
Fortunately scarring doesn’t occur in SSSS as the splitting of the epidermis occurs intradermally not subdermally (as in TEN) so parents can be reassured that their baby won’t be scarred for life as a result of the infection however horrendous the skin looks.
How is SSSS diagnosed?
The main method of diagnosis is clinical. It is very distinctive. It is important to make sure the S. aureus hasn’t spread anywhere else, so blood cultures should be taken as well as skin swabs from involved areas of skin. DO NOT use a single swab moving from lesion to lesion, use a single swab for each individual area of broken skin; if one area of skin is infected (usually secondary infection) and you swab this area and then move to other areas you will spread the infection to all of them! Remember the skin lesions of SSSS are normally sterile, the bacterium is somewhere else releasing toxin into the body not in the skin itself.
If it is critical to distinguish SSSS from TEN then a biopsy can be taken for histology to look where the epidermis is being split, but this is rarely required.
How is SSSS treated?
Children with SSSS often need to be admitted to hospital for assessment, as the area of broken skin can be extensive and fluid balance can be a problem. Some of these children require IV fluids as part of their initial care.
Intravenous antibiotics targeting S. aureus should be started as soon as possible and when the child has started to improve they can be switched to oral antibiotics, for a total of 10 days. However, older children who are eating and drinking well can often be treated just with oral antibiotics.
1st line |
IV Flucloxacillin |
2nd line (if 1st line contraindicated) |
IV Clindamycin |
If high prevalence of community MRSA* |
IV Teicoplanin OR IV Vancomycin |
The broken areas of skin should also be protected with emollients such as ointments or creams to help keep them moist and prevent secondary infection. These will also help reduce the pain as it is often air getting to the area of broken skin that triggers the pain response.
Pain relief with Paracetamol is often required but non-steroidal inflammatory drugs e.g. Ibuprofen should be avoided as they can impair renal function and potentially make the infection worse.
If treated promptly and effectively SSSS is not usually fatal in children (mortality <5%) although in adults the mortality is said to be higher usually because there is some underlying immunosuppression in this patient group.
Infection control
All children with SSSS should be isolated in a single room. Good hand hygiene is essential as there is a high outbreak potential of this type of infection in hospitals, nurseries and schools. It is also good practice to wear gloves and aprons to protect yourself when caring for these children in hospital.
So our baby was admitted to the ward and started on IV Flucloxacillin whilst his mother was made a strong cup of tea. Two days later the baby’s skin was looking much better and they were changed to oral Flucloxacillin and allowed to go home. Later that afternoon the skin swab results came back showing the presence of S. aureus. Both the mother and her baby made full recoveries and neither had long term scars.

 RSS Feed
RSS Feed
