The stool samples were negative but a week later another phone call came through to the Microbiologist, this time from the London Hospital for Tropical Diseases laboratory saying the patient had tested positive for strongyloidiasis. The Microbiologist phoned the GP to give him the good news and explain how to treat the patient. The GP was thrilled, and revealed that they had read about the diagnosis and would explain it all to the patient, including the life-cycle and how it’s acquired. With some reservations the Microbiologist hung up the phone, not sure that the patient would really want to know all of this information.
What is strongyloidiasis?
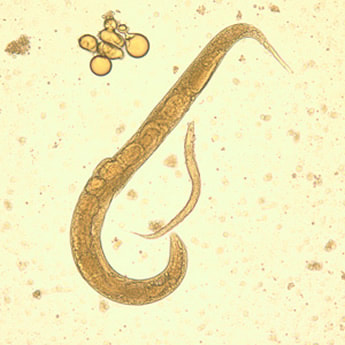
Strongyloidiasis is a tropical and sub-tropical parasitic infection, with prevalence rates as high as 25% in some parts of the World. The cause is a parasite called Strongyloides stercoralis. Infection occurs when the tiny filariform larvae enter through the skin from soil contaminated with human faeces. The larvae then travel through the bloodstream to the lungs where they “hatch” out into the alveoli, before being coughed up and swallowed again. During this process the adult worms mature, burrowing into the lining of the duodenum and jejunum where they release eggs which become filariform larvae and the whole cycle begins again!
How does strongyloidiasis present?
The majority of patients with strongyloidiasis are asymptomatic however others present with skin, gastrointestinal or respiratory symptoms. Another reason for making the diagnosis is the incidental finding of eosinophilia in a patient’s peripheral blood. The most severe form of infection is known as hyperinfection syndrome.
Eosinophilia: levels of eosinophils ≥ 5 x 108/L are usually considered abnormal and ≥ 50 x 108/L is considered severe. Depending on where the patient is from affects how likely the cause is to be parasitic; other causes include cancer, drug reactions and autoimmune diseases. Strongyloidiasis is the most common parasitic infection causing eosinophilia although others include toxocara, trichinella, schistosomiaisis, filariasis (e.g. with Loa loa), ascariasis, hookworm and intestinal flukes… maybe these should be future blogs!?
Skin reactions: some patients get intense itching and swelling at the point where larvae penetrate the skin. As the larvae spread through the body they may leave a raised pink track known as larva curens (running larva). The presence of larva curens is diagnostic for strongyloidiasis.
Gastrointestinal symptoms: adult worms cause inflammation of the duodenum with abdominal pain. Diarrhoea, vomiting and anorexia are common. Very high burdens of worms can cause malabsorption.
Respiratory symptoms: larvae penetrating into the alveoli can cause a dry cough, shortness of breath, wheeze and occasionally haemoptysis. This can mimic Loeffler’s syndrome which is seen with ascariasis. Severe infections can present as asthma, recurrent pneumonia or chronic obstructive pulmonary disease. Treating the parasite makes the respiratory illness disappear.
Hyperinfection syndrome: massive numbers of larvae penetrate various body organs such as the lungs, liver, heart, central nervous system and endocrine glands. This can lead to irreversible damage to these organs and even cause septic shock as Gram-negative bacteria penetrate through the inflamed bowel wall. Hyperinfection syndrome more often occurs with autoinfection or immunosuppression (e.g. steroids, congenital immunodeficiency, alcoholism or malnutrition). Hyperinfection syndrome presents with fever, nausea, vomiting, diarrhoea, abdominal pain, shortness of breath, wheeze, cough and haemoptysis (basically a mixture of the other types of presentation above). Other symptoms are related to the body organs involved e.g. meningitis or liver failure. The mortality of hyperinfection syndrome can be as high as 80%!
How do you diagnose strongyloidiasis?
Okay, so the life cycle is quite disgusting and severe disease can kill your patients, so how do you know if they have it? It is sometimes possible to see larvae in stool samples as well as duodenal aspirates and even sputum, but the sensitivity of stool microscopy is less than 50% because larvae are only excreted intermittently.
In the UK we tend to rely on serology using an ELISA to detect IgG against the filariform larvae. Some patients who test positive for strongyloidiasis actually have ascariasis or hookworm, as these two parasites can give a false positive strongyloidiasis test. It is therefore advisable when sending serology for strongyloidiasis to send stool samples to exclude ascariasis and hookworm. It is also possible to get false negative tests in immunosuppressed patients, especially those who have problems with producing IgG.
How do I get rid of the wee beastie?
Fortunately the treatment of strongyloidiasis is relatively simple. The main problem is trying to get hold of the drugs as they are not normally stock items for UK pharmacies and can occasionally be in short supply.
Initial therapy |
Antibiotic |
1st Line |
PO Ivermectin 200mcg/kg OD for 2 days |
2nd line (if 1st line contraindicated) |
PO Albendazole 400mg BD for 7 days |
Whatever the treatment used in any of the presentations of strongyloidiasis, the patient should be followed up with repeat full blood counts (for eosinophilia), stool samples and serology (at 1, 3,6 and 12 months after treatment) to make sure they don’t relapse. If the patient is cured the eosinophil count should return to normal within 3 months and serology should reduce significantly after 6 to 12 months, although it is unlikely to become negative as it is an IgG response and therefore may persists long-term. If the tests do not suggest cure then the patient should be retreated with the same regimen above.
How do people protect themselves from developing strongyloidiasis?
Okay, this may sound very simple, but the best way to prevent the acquisition of S. stercoralis from contaminated soil is to wear shoes. Yep shoes! The most common area of the body where the larvae penetrate the skin is the feet, therefore shoes are the best protection, even if they only cover the sole such as those made from old car tyres and worn in rural areas of Africa. A simple message: protect the skin and prevent the infection.

 RSS Feed
RSS Feed
