annually; more than breast cancer and bowel cancer combined”1. Back in 2005 the Surviving Sepsis Campaign attempted to rectify this by raising awareness and improving the management of septic patients with evidence based
guidelines. However these guidelines are, “delivered in fewer than 1 in 5 [septic] patients in the UK”1.
So could you recognise a patient with sepsis and reel-off an initial management plan? No?
Sepsis is a clinical diagnosis not a laboratory test. It requires the doctor to make the diagnosis. Sepsis is infection with evidence of the systemic response to that infection e.g. hypoxia, oliguria, confusion. Severe sepsis is sepsis with organ dysfunction, hypoperfusion or hypotension. “Sepsis is better thought of as the body’s severe response to an infection rather than a severe infection”1. Sepsis is life threatening and an emergency. The recognition of the septic patient is one of the key skills a medical student or junior doctor needs to learn.
Often when I ask medical students and junior doctors what the criteria are for diagnosing sepsis I get told it’s based on the Modified Early Warning Score (MEWS) or Paediatric Early Warning Score (PEWS) but this is not the case. These scoring systems are designed to help other ward staff, such as nurses, recognise a deteriorating patient and empower them to call medical support. It doesn’t make sense for the arriving doctors to then use the same tool to try and decide why the patient is unwell. Early warning scores (see images below) are essentially a numerical value assigned to the physiological parameters on the observation chart, i.e. they quantify the observations. Sepsis is just one reason why a patient may have a high MEWS or PEWS score. It is the doctor’s job to try and work out what the diagnosis is.
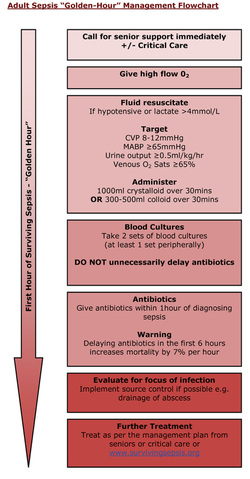
These questions should be asked and investigated as rapidly as possible in order to try and give appropriate antibiotics within the first 45-60 minutes “The Golden Hour” see flowchart below. The antibiotics chosen should cover the common bacteria such as Staphylococcus aureus, Enterobacteriaceae, Pseudomonas sp. as well as Neisseria meningitidis in younger patients (usually < 18 years old).
The other key aspects of the management of sepsis are to provide oxygen, fluid resuscitation and identify and treat (surviving sepsis call this “source control”) the underlying cause of the sepsis such as an UTI, abscess or intra-abdominal perforation. See clinical scenarios, Sepsis for further information.
Remembering the full guidelines can be complex and requires collaboration between A&E, ward and ITU doctors,
but the initial management can be simplified to six steps, now commonly known as the “Sepsis Six”. Try the mnemonic “SEPTIC” to remember them:
- Start high-flow oxygen
- Extract blood cultures
- Prescribe and give empiric antibiotics
- Take lactate and send full blood count
- IV fluid resuscitation
- Check urine output
given a 20-30% better chance of surviving sepsis1.
It is one thing for a patient to die when you have recognised how unwell they are and done everything possible to try and save their life. This is unfortunately one of the hard truths of medicine. But it is another, unacceptable thing, for a patient to die because someone failed to recognise how unwell they were and failed to take the necessary steps to manage them properly. All medical students and junior doctors should become familiar with the surviving sepsis guidelines in order to try and prevent avoidable deaths from sepsis.
The Surviving Sepsis campaign published new guidelines in 2012 http://www.survivingsepsis.org/Guidelines/Pages/default.aspx
Ref 1 http://sepsistrust.org/



 RSS Feed
RSS Feed
