very topical given the recent publication of the Chief Medical Officers report on antimicrobial resistance as well as a
Department of Health five year strategy for combating antimicrobial resistance.
significant point; humans don’t have to develop an infection with these resistant animal bacteria, for there to be a problem. The organism may not matter, but its resistance mechanism does.
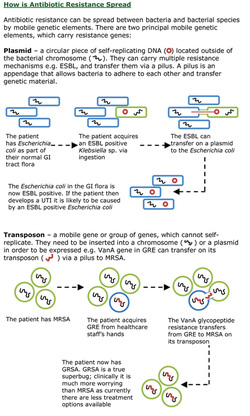
slugs and snails!). It is not the organism that causes the problem but rather the transfer of the resistance genes on a mobile genetic element (in this case a plasmid – see image) from a non-pathogenic bacteria (Kluyvera) to a pathogenic one (E. coli).
So, as a microbiologist am I worried by antibiotic use in animals?
Bacteria are evolving resistance faster than we can produce new antibiotics. There have been extensive bacteria resistant to the antibiotics within the last 20 years e.g.
• Escherichia coli (Cephalosporin, Gentamicin &
Ciprofloxacin resistance)
• Staphylococcus aureus (Flucloxacillin resistance)
• Enterococcus faecium (Vancomycin resistance)
• Neisseria gonorrhoea (Ciprofloxacin resistance)
• Acinetobacter iwofii (Meropenem resistance)
• Pseudomonas aeruginosa (Meropenem, Ciprofloxacin &
Gentamicin resistance)
• Streptococcus pneumoniae (Penicillin & Ceftriaxone resistance)
This list isn’t exhaustive but these bacteria are resistant to 6 of the 16 types of antibiotics available; in contrast there has been only one completely new antibiotic class in the same time period. If we don’t take better care of our antibiotics, we will be back in a pre-antibiotic era where 10% of patients with skin infections and 60% of patients with pneumonia died as no treatment will be available.
 RSS Feed
RSS Feed
